 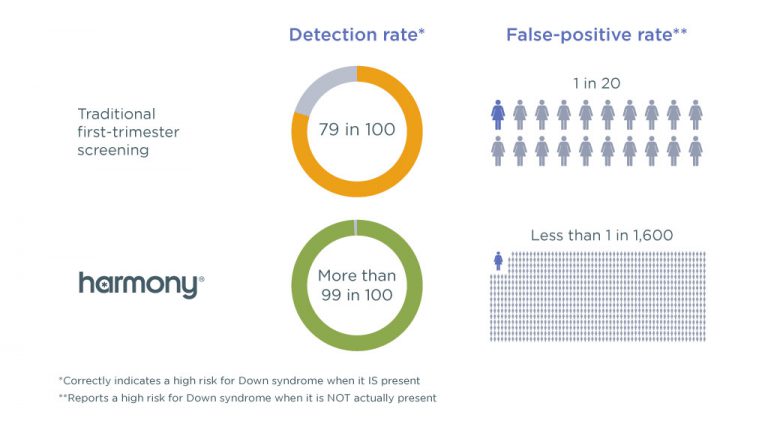
In 2018, NIPT will be introduced for the screening of trisomies. It has been proven possible to sequence the whole fetal genome from cfDNA, but it is currently too time consuming and costly to do routinely. This is referred to as NIPD – non-invasive prenatal diagnosis. In these instances the result is definitive and does not need to be confirmed by invasive tests. The technique has also now been adapted to some rare genetic diseases that are caused by single gene variation, including cystic fibrosis and Apert syndrome. Sex chromosome aneuploidies such as Turner syndrome ( monosomy X) and Kleinfelter Syndrome (XXY) are also detectable. The test is primarily used to detect aneuploidies – where an abnormal number of chromosomes is present in each cell – specifically the trisomies that cause Down’s, Edwards’ and Patau’s syndromes.Īs fetal sex is determined by chromosomes, accurate sex determination is also possible from nine weeks gestational age – much earlier than by ultrasound.  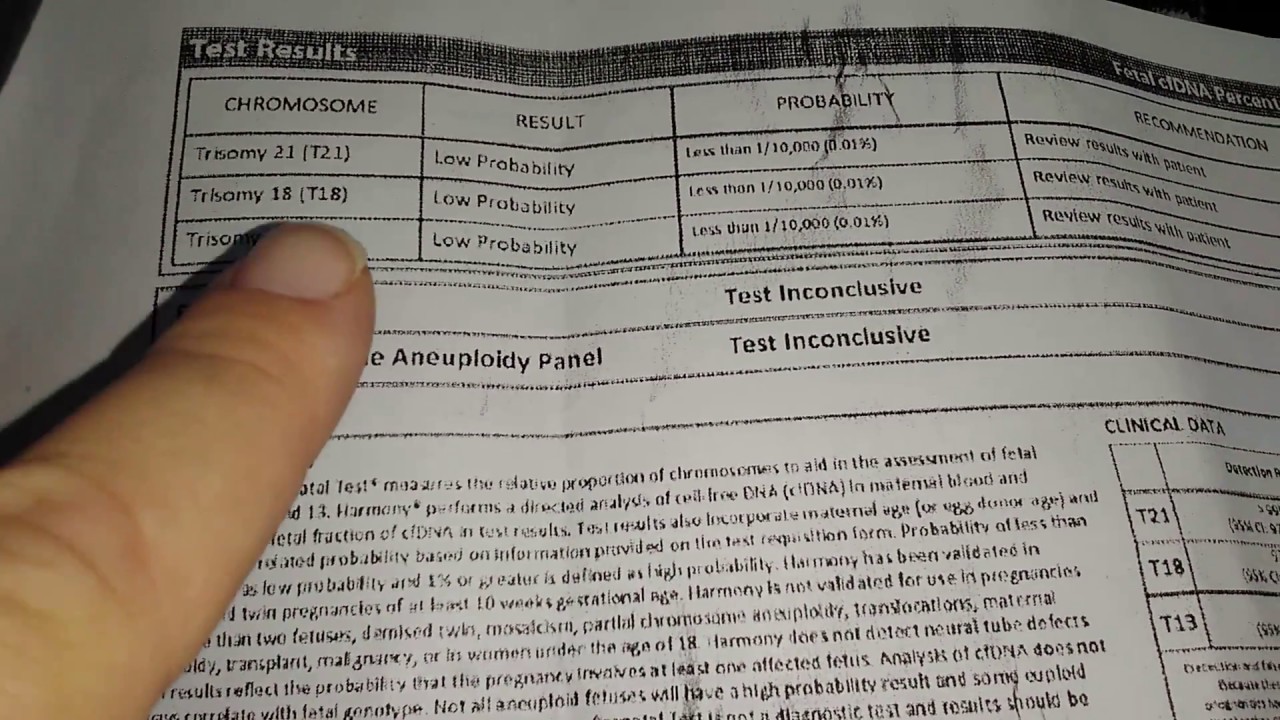
The fragments can also be tested for specific genetic markers. By looking at the proportions of fragments it is possible to determine if they come from a person with the standard complement of 46 chromosomes, or if there are more or fewer. Most of these fragments will be from the mother, but a proportion will come from the placenta and therefore carry the DNA of the fetus.įrom blood, the cfDNA can be isolated and examined for a range of abnormalities, and it is possible to identify which chromosome each fragment comes from. NIPT works by examining the small fragments of DNA – known as cell free DNA (cfDNA) – floating in the mother’s blood. Other prenatal tests draw inferences from ultrasound scans and the hormone levels of the mother to predict the likelihood of a range of conditions, but these are not genetic tests and can only indicate risk rather than provide a reliable diagnosis. Both also increase the risk of miscarriage by around one percent, and are therefore only used when other measures show a high risk of disease or abnormality. Both of these methods involve collection from inside the uterus and are considered invasive. Previous techniques for prenatal genetic testing involved taking a sample of fetal cells, either from the placenta (a process known as chorionic villus sampling or CVS) or from cells shed by the fetus into the amniotic fluid ( amniocentesis). Next year, the health service will be offering testing to women identified as having a high risk of an affected pregnancy – meaning their unborn child is at risk of having a serious health condition. Non-invasive prenatal testing (NIPT) is a way of examining fetal DNA by taking a sample of blood from a pregnant woman. But how does it work? And what are the benefits? Non-invasive prenatal testing will be rolled out in the NHS next year. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
